Atrial fibrillation, often called AFib, is the most common type of irregular heartbeat, affecting millions worldwide. This condition occurs when the heart’s electrical signals become chaotic, causing the upper chambers to beat out of sync with the lower ones. While it may seem harmless at first, untreated AFib can significantly increase the risk of stroke and other heart-related complications.
Recognizing the signs and understanding the causes of AFib are crucial for managing it effectively. From a racing heartbeat to unexplained fatigue, the symptoms can vary widely, making early detection essential. Fortunately, advancements in medical treatments and lifestyle adjustments offer hope for those living with this condition.
Understanding Atrial Fibrillation: What Causes Irregular Heartbeats?
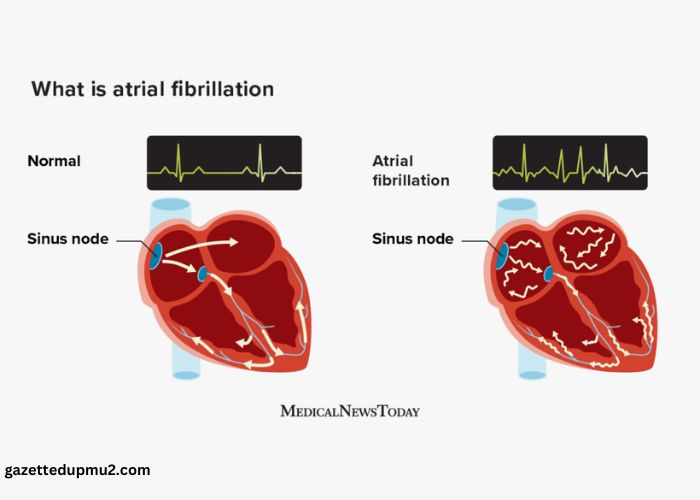
Atrial fibrillation occurs due to disruptions in the heart’s electrical signals, leading to an irregular or rapid heartbeat. Electrical impulses, originating in the sinoatrial (SA) node, control the heart’s rhythm. In AFib, abnormal signals interfere with this process, causing the upper chambers (atria) to beat chaotically.
Structural changes in the heart are a major cause. Conditions like high blood pressure and coronary artery disease can damage the heart’s structure, increasing the risk of AFib. Valve disorders, such as mitral valve prolapse, also contribute by altering blood flow and placing added strain on the atria.
Lifestyle factors impact AFib development. Heavy alcohol consumption, chronic stress, and obesity disrupt the heart’s electrical activity. Sleep apnea, another risk factor, deprives the heart of adequate oxygen, intensifying arrhythmias.
Chronic illnesses often lead to AFib. Diabetes, hyperthyroidism, or lung conditions like chronic obstructive pulmonary disease (COPD) can indirectly trigger irregular heartbeats. Aging also raises susceptibility, as the cardiovascular system weakens over time.
Genetics play a role in certain AFib cases. People with a family history of arrhythmias may carry inherited traits that disrupt normal heart rhythms. Tap here to learn more about managing atrial fibrillation and your heart health.
The Most Common Symptoms of AFib and When to Seek Medical Help
Atrial fibrillation symptoms vary but often disrupt normal daily activities. Palpitations, where the heart feels like it’s racing or fluttering, are a leading sign. Irregular heartbeats may last from minutes to hours, affecting concentration and rest.
Fatigue is another prominent symptom. It can occur even after minimal exertion due to the heart’s inefficient blood pumping. Many individuals also report weakness, dizziness, or feeling faint, particularly during physical activity.
Breathlessness, especially during exertion or while lying down, frequently accompanies AFib. Swelling in the legs or feet can develop if the condition remains unmanaged, signaling worsening heart function.
Chest pain could signify reduced blood flow caused by irregular rhythms. Immediate evaluation is essential if chest pain occurs, as it may mimic or indicate a heart attack.
Seek medical help if these symptoms disrupt daily life or if chest pain, severe dizziness, or fainting happens. Early detection and specialized care improve long-term outcomes, significantly reducing stroke and complication risks.
How AFib Increases the Risk of Stroke and Other Complications
Atrial fibrillation disrupts normal blood flow, leading to the formation of blood clots. In AFib, irregular heartbeats cause the atria to quiver instead of contracting effectively. As a result, blood can pool in the atria, particularly in the left atrial appendage, forming clots that may travel to the brain and block blood flow, causing a stroke.
Strokes caused by AFib are often more severe. According to the Centers for Disease Control and Prevention (CDC), individuals with AFib face a fivefold increase in stroke risk. The severity of AFib-related strokes often leads to long-term disabilities or higher mortality rates compared to strokes from other causes.
AFib heightens the risk of heart-related complications. Prolonged periods of irregular heart rhythms strain the heart, potentially causing heart failure. This condition arises when the heart becomes too weak to pump sufficient blood to the rest of the body, resulting in fatigue, swelling, and shortness of breath.
Other complications include cognitive decline and blood vessel-related damage. Studies link AFib to an elevated risk of dementia, even in those who haven’t suffered a stroke. Inflammation from clots and poor blood circulation may contribute to damage in other organs, worsening overall health outcomes.
Managing underlying risk factors aids in reducing complications. Lifestyle changes, such as minimizing alcohol consumption and controlling high blood pressure, alongside anticoagulant medications, significantly lower the chances of strokes and heart-related issues in AFib patients.
The Role of Lifestyle Changes in Managing Atrial Fibrillation
Lifestyle modifications play a critical role in managing Atrial Fibrillation Basics (AFib) and reducing its complications. By addressing key risk factors, these changes help regulate heart rhythm and improve overall health.
Weight Management
Maintaining a healthy weight reduces AFib episodes and supports heart function. Studies show that a 10% reduction in body weight can significantly decrease arrhythmia severity. Obesity amplifies atrial strain, so a balanced diet and regular exercise are essential.
Diet and Nutrition
A heart-healthy diet minimizes AFib risks. Dietary approaches like the Mediterranean diet, rich in fruits, vegetables, whole grains, and healthy fats, lower inflammation and aid heart rhythm stability. Limiting salt reduces blood pressure, further decreasing AFib triggers.
Physical Activity
Moderate exercise enhances cardiovascular health and lowers AFib frequency. Activities like walking or cycling improve circulation and maintain a healthy weight. However, excessive high-intensity exercise may exacerbate AFib episodes for some individuals.
Alcohol Consumption
Reducing alcohol intake benefits those with AFib. Heavy drinking (more than seven drinks weekly) heightens AFib risk by causing electrical imbalances in the heart. Abstinence or moderate consumption helps maintain rhythm regularity.
Stress Reduction
Stress management techniques alleviate AFib symptoms. Practices such as yoga, meditation, and deep breathing lower cortisol levels and stabilize heart rate. Chronic stress often exacerbates AFib by increasing sympathetic nervous system activity.
Sleep Quality
Treating sleep disorders like sleep apnea decreases AFib recurrence. Sleep apnea disrupts oxygen levels, causing structural heart changes. Using CPAP therapy or improving sleep hygiene promotes better cardiac outcomes.
Lifestyle adjustments, combined with medical treatments, provide a comprehensive approach to AFib management. Making these changes can significantly reduce reliance on interventions and improve long-term quality of life.
Medications Used to Control AFib and Prevent Blood Clots
Medications play a central role in managing atrial fibrillation by controlling heart rhythm and reducing stroke risk. Physicians base treatment approaches on the severity of AFib, underlying conditions, and the risk of complications.
Heart Rate and Rhythm Control Medications
Heart rate control ensures that the heart beats at a healthy pace. Commonly prescribed drugs include beta-blockers, like metoprolol, and calcium channel blockers, such as diltiazem. For rhythm control, anti-arrhythmic drugs help restore a regular heartbeat. Examples of these include amiodarone and flecainide. These medications aim to improve symptoms and prevent worsening heart dysfunction.
Anticoagulants to Prevent Blood Clots
AFib increases the likelihood of forming blood clots in the heart. Anticoagulant medications lower the risk of stroke by preventing clot formation. Direct oral anticoagulants (DOACs) like apixaban and rivaroxaban are commonly used due to fewer dietary restrictions and monitoring requirements. Warfarin remains an option but requires regular blood tests to manage its effects. These drugs are particularly important for patients at higher stroke risk based on scores like CHA2DS2-VASc.
Additional Considerations for Treatment
Anti-platelet medications, such as aspirin, may be prescribed for individuals with low stroke risk, though they are less effective than anticoagulants. Combination therapy might be necessary for select cases but raises bleeding risk. Regular follow-up visits ensure dosage adjustments and minimize side effects tied to long-term medication use.
Medications, paired with lifestyle adjustments and regular monitoring, provide an effective strategy for managing AFib and preventing related complications, including blood clots and heart failure.
Advances in Catheter Ablation and Other AFib Treatments
Catheter ablation is a groundbreaking treatment for atrial fibrillation that targets erratic heart rhythms. This minimally invasive procedure uses heat (radiofrequency) or cold (cryoablation) energy to destroy areas of heart tissue causing abnormal electrical signals. Studies indicate success rates of 70-80% for achieving long-term heart rhythm control, particularly in patients with paroxysmal AFib. Advanced imaging and mapping technologies have refined the accuracy of ablation, improving outcomes and reducing recurrence rates.
Hybrid ablation merges catheter ablation with minimally invasive surgical techniques. This innovative approach enhances success rates in persistent or longstanding AFib cases. It enables precise treatment of areas inaccessible through traditional methods.
Maze surgery, a more invasive but highly effective option, benefits patients who don’t respond to other treatments. Surgeons create scar patterns in the atria to block irregular electrical signals, restoring normal rhythm.
Increasing use of left atrial appendage closure devices offers additional stroke prevention in patients unable to tolerate anticoagulants. Devices like the Watchman reduce stroke risk by sealing off the appendage, which is a common site for clot formation in AFib.
Anti-arrhythmic drugs and rate-controlling medications complement these procedures, particularly for individuals not pursuing or not responding to ablative techniques. Combining pharmacological therapy with interventions creates a comprehensive treatment plan tailored to individual needs. Advanced treatment options have revolutionized AFib care, aligning it with modern medical innovations.
The Connection Between AFib and Other Heart Conditions
AFib frequently coexists with or arises due to other heart conditions. These associations complicate both diagnosis and management, impacting overall heart health. Understanding these links is crucial for effective treatment strategies.
- Hypertension: High blood pressure leads to structural changes in the heart, like left atrial enlargement, increasing AFib risk. Up to 60% of people with AFib also have hypertension.
- Coronary Artery Disease (CAD): CAD limits blood flow to the heart, weakening heart muscles and disrupting electrical pathways, often triggering AFib. Studies indicate co-occurrence in 17% of AFib patients.
- Heart Failure: AFib and heart failure share a bidirectional relationship. AFib weakens heart efficiency, while failing hearts can develop rhythm abnormalities. About 30-50% of heart failure patients develop AFib.
- Valvular Heart Disease: Defective heart valves, such as those in mitral stenosis or regurgitation, alter blood flow dynamics, stressing heart chambers. Valvular AFib typically presents more severe symptoms.
- Congenital Heart Defects: Structural anomalies present from birth, like atrial septal defects, predispose individuals to AFib. This correlation is increasingly observed as congenital heart defect patients live longer.
- Myocarditis and Cardiomyopathy: Inflammation or disease of the heart muscles, as in myocarditis or dilated cardiomyopathy, disrupts regular electrical activity. Both conditions substantially elevate AFib risk.
Addressing these underlying heart issues often stabilizes or improves AFib outcomes. Combined management approaches tailored to individual needs mitigate complications and enhance recovery rates.
How Wearable Technology Helps Monitor AFib Symptoms in 2025
Wearable technology has become a game-changer in managing atrial fibrillation. Devices like smartwatches and fitness trackers now offer advanced features such as continuous heart rate monitoring, irregular rhythm detection, and ECG capabilities. These tools empower individuals to track their heart health in real time and identify potential AFib episodes early.
The ability to share data with healthcare providers ensures timely interventions and personalized treatment adjustments. As technology continues to evolve, wearables are expected to play an even greater role in AFib care, bridging the gap between patients and providers while enhancing overall disease management.